
Getting a diagnostic mammogram can be a stressful experience. You might have a diagnostic mammogram after an abnormal finding in your regular screening mammogram, or because you noticed some new or unusual symptoms in your breast. But a diagnostic mammogram doesn’t always equal bad news. Almost 50% of women who get annual mammograms will experience at least one false positive over a ten-year period.
Knowing why a diagnostic mammogram is ordered and what to expect can relieve some of that tension. This post will examine:
A diagnostic mammogram is a type of X-ray that uses a low dose of radiation to take images of breast tissue. Mammograms are the most common screening test for breast cancer, which is the second-most common source of cancer in women in both the U.S. and Canada.
Screening mammography monitors changes in breast tissue and detects early signs of breast cancer, often long before you feel any sort of symptoms. In 2023, the U.S. Preventative Services Task Force issued draft recommendations that women should begin receiving screening mammograms every other year starting at age 40.
There are several types of mammograms:
A screening mammogram is a regular scan in which images are taken of both breasts to check for signs of disease in patients exhibiting no symptoms. Doctors use baseline mammograms to monitor changes in breast tissue over time. Mammograms can identify abnormal areas before you feel any signs or symptoms. According to the National Cancer Institute, mammograms are the most common screening test to detect breast cancer.
A diagnostic mammogram is performed to diagnose a specific area, lump or problem in the breast. The process takes a little longer than a screening mammogram, and will usually cover both breasts for comparison purposes. The radiologist or interpreting physician may be present, and any follow-up imaging may be taken right away.
Having a diagnostic mammogram does not mean you’ll be diagnosed with cancer. According to a recent study of more than one million participants, 10.3% of women are recalled for further imaging after a regular digital screening mammogram in order to get more information. There are several reasons a doctor might order a diagnostic mammogram, including:
The American Cancer Society estimates that almost 298,000 women will be diagnosed with breast cancer in 2023. Health Canada notes that 82% of those cases will be detected early, in stage 1 or 2. The 5-year survival rate for breast cancer is 96.3%.
The mortality rate for breast cancer has dropped dramatically since 1989, down 43% by 2020. Screening and diagnostic mammograms lead to earlier detection, which makes for more positive health outcomes overall.
There are some steps you can take to prepare for your diagnostic mammogram procedure:
The imaging clinic or department will provide wipes to clean up after your screening, but you may wish to pack deodorant or antiperspirant to bring with you to wear after the appointment. Also, if you are concerned about pain during your appointment, ask your doctor if over-the-counter medication can help reduce discomfort.
The technician is not allowed to answer questions about the results of your diagnostic mammogram. But feel free to ask questions about the process and procedure, including:
Afterward, the radiologist will review and interpret your results, forwarding a full report to your referring physician. At your follow-up appointment, you can ask your doctor more specific questions, like:
Your mammogram results are interpreted by a radiologist—an expert in medical imaging—who carefully reviews your scans and provides a detailed report of any findings. This report is then sent to your referring physician, who, with a deeper understanding of your medical history and past exams, can offer further insights and recommendations on next steps in a follow-up appointment.
Turnaround times for imaging results can vary widely depending on the facility and your doctor’s availability. Often, patients wait a week or more and receive their results during a follow-up appointment. With PocketHealth, your imaging results are securely accessible as soon as they’re approved for release by the hospital or imaging clinic. This allows you the opportunity to review your results and prepare questions ahead of your follow-up visit.
To help you understand your mammogram results, PocketHealth provides clear definitions and illustrations for complex medical terms—plus an in-depth explanation of your full imaging report. This is paired with highlights of key anatomy in your imaging to help you better comprehend what you’re looking at.
In a diagnostic mammogram image, your breast tissue shows up in shades of gray against a black background. Dense breast tissue and glands appear white. Calcium deposits, or calcifications, are visible as white flecks of various sizes. Cysts are fluid-filled structures with thin outer walls.
A tumor will appear as a concentrated white shape. Having a tumor does not mean you have cancer. Fibroadenomas are benign tumors that tend to shrink as you age, so they’re more common among women in their 20s and 30s.
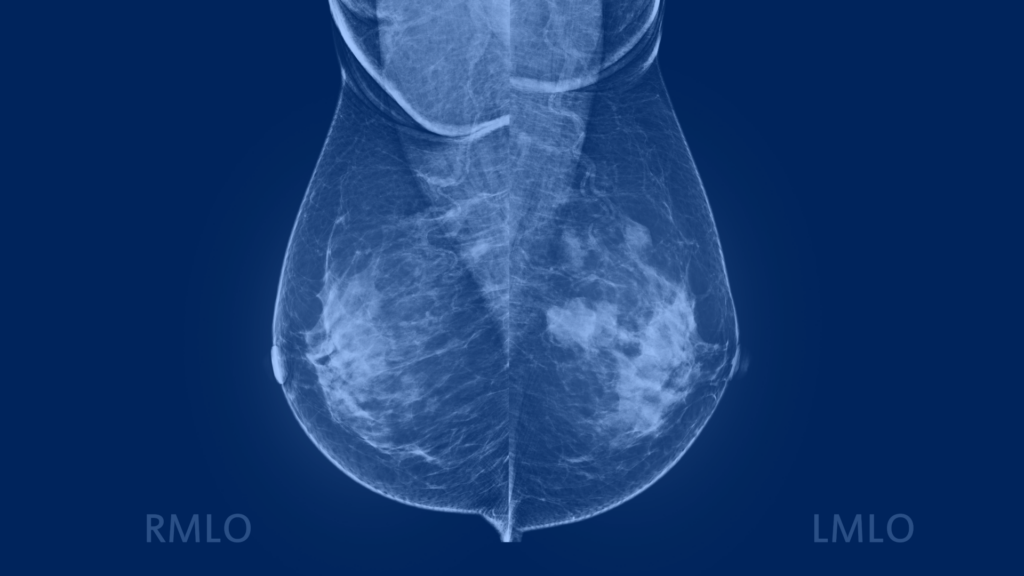
A mammogram image showing malignant tumors in both breasts, which are categorized as BI-RADS category 4.
A diagnostic mammogram is used to clarify a previous finding or to examine areas presenting symptoms. It can illuminate calcifications, explore masses, or measure asymmetries. None of those findings automatically mean cancer.
Doctors use a specific standard vocabulary to explain mammogram results, called the Breast Imaging Reporting and Data System (BI-RADS). BI-RADS has seven numbered categories:
Many findings, like cysts and fibroadenomas, are normal occurrences. Findings can generally be divided into 3 categories:
Depending on the BI-RADS results of your diagnostic mammogram, you may need some further testing to assess or diagnose cancer or other conditions, such as:
If you do get a cancer diagnosis, these tests will provide more information about the cancer’s type and severity. The test results, along with the symptoms you’re experiencing, will help your doctor decide which treatment options might be best for you.
With PocketHealth, it’s simple to keep track of your all your mammogram results. All of your images and reports are permanently available in one secure location and can be accessed online—anytime, anywhere. Reports can also be easily shared with other members of your care team, if needed. When used in conjunction with your medical provider’s professional advice, it is a powerful tool to better understand your imaging results.
PocketHealth also provides personalized health insights based on the findings in your report to help you stay on top of any next steps. This includes clearly surfacing any follow-up actions found in your report and generating customized questions to ask your doctor so you can make the most of your follow-up appointment.
The last three decades have witnessed a substantial drop in breast cancer mortality among women, largely due to effective early screening. Regular screening mammograms and diagnostic mammograms are highly efficient detection measures that can catch breast cancer at its earliest stages.
If you’re located in Ontario, you’ll have the option to get your breast cancer risk score and determine your eligibility for Ontario Breast Screening Program (OBSP), as part of PocketHealth’s suite of breast health tools. If you’re eligible for OBSP, you can even book your next mammogram directly through PocketHealth.
Not every finding in a diagnostic mammogram is cancer. However, the earlier cancerous and precancerous findings are caught, the easier they are to treat and the higher the survival rate.
If you have breast cancer and are looking for more information, the following resources may help:
Learn more about how to use PocketHealth to access and share your mammogram records.
Published: September 5, 2023
Trusted by more than 900+ hospitals and clinics.











