Types of Breast Screening Exams: Self, Mammogram and More
Aside from non-melanoma skin cancer, breast cancer is the most common cancer for patients assigned female at birth (AFAB), with an estimated 1 in 8 developing the disease in their lifetime. There are multiple techniques to screen for this disease, which this guide will cover in detail.
For those looking to take proactive control of their breast health, PocketHealth can help. With secure, easy access to your breast imaging records, PocketHealth allows you to understand your breast health better. In addition, PocketHealth offers personalized estimated breast cancer risk scores to help you and your doctor make informed decisions about preventive measures and future screenings.
Breast cancer screening recommendations
In previous years, the recommended age for breast cancer screening was 50 to 74, but it has since been lowered to 40. Currently, patients at average risk for breast cancer receive a mammogram every two years. Those at higher risk may be advised to undergo screenings more frequently or to use alternative or additional screening methods.
The main reason for this change is to detect breast cancer earlier, when treatment is most effective and the survival rate is nearly 100 percent. Additionally, research has shown that Black patients have a 40 percent higher mortality rate from the disease, meaning earlier screenings can save lives and detect aggressive cancers at an earlier stage.
Types of breast exams
There are several breast exam methods, each with its own strengths. These include:
- Breast self-exams
- Clinical breast exams
- Mammograms
- Breast ultrasounds
- Breast MRIs
- Digital breast tomosynthesis
Medical providers may recommend different techniques, or a combination of them, based on the patient’s risk factors and family history.
Breast self-exam
There is currently mixed opinion among healthcare professionals regarding whether this type of exam is still recommended, with some claiming that mammograms and similar screenings are sufficient, while others continue to value self-exams as a useful complementary method. The reasoning against self-exams is that they can lead to false positives (as most breast lumps are non-cancerous) and result in unnecessary screenings, biopsies and stress. You may want to ask your healthcare provider for guidance, as many doctors still recommend continuing this practice, and staying familiar with your breasts can help you notice any changes or abnormalities.
In terms of how it works, this is the simplest breast exam, as it is quick and can be done at home. If it is determined you should utilize this method, perform the examination monthly to feel for lumps or breast changes. The self-exam should supplement other screening methods and be used in addition to examinations like mammograms.
How to perform a breast self-exam
Patients who still menstruate should perform the exam a few days to a week after their cycle ends, when breast changes are minimal. Non-menstruating patients should choose a specific day each month, such as the 16th, and repeat the exam on the same date each month. Performing the exam regularly not only helps track changes but also allows patients to become familiar with their breasts so they can better notice irregularities.
To perform the breast self-exam:
- Stand in front of a mirror and visually examine your breasts: Begin with your arms by your sides and your chest relaxed. Look for any changes in shape, symmetry, inverted nipples or signs of dimpling or puckering. Repeat the inspection with your hands on your hips, flexing the chest muscles, and once more with your arms raised overhead.
- Feel for breast changes or lumps in the shower: Using the pads of your index, middle and ring fingers, apply varying pressures to all areas of both breasts and your armpits. Take your time, follow a systematic pattern and check for lumps, hard areas or thickening.
- Feel for breast changes or lumps while lying down: Lie on your back in a comfortable position, placing a pillow beneath one shoulder and raising the arm of that side behind your head. With the opposite hand, gently press down with varying pressures on your breast and armpit area using the pads of your middle three fingers. Switch the pillow to the other shoulder and repeat the steps on the other side. Also, gently squeeze each nipple to check for discharge.
Patients with physical restrictions or reduced range of motion may wish to ask their doctor for alternative breast self-exam techniques, so they can perform this exam more comfortably. If any lumps or abnormalities are discovered, patients should inform their doctor, who may have them undergo breast imaging scans.
Clinical breast exam
Clinical breast exams are similar to breast self-exams, except they are performed by a physician during your doctor’s appointment. Recommendations for these exams are also mixed, with many healthcare professionals claiming they have limited value when more detailed screening methods are available. However, clinical breast exams are still commonly performed at a doctor’s visit, especially if the person is at higher risk for breast cancer or feels a potential lump on their own.
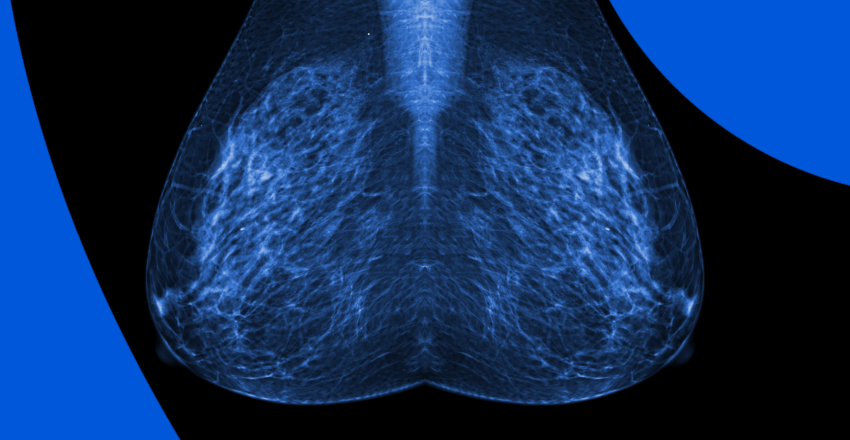
Mammogram
Mammograms, or low-dose X-rays, are the most common screening exams for those with an average risk for breast cancer. Those with high risk may be asked to get a mammogram and breast MRI. During a mammogram exam, your breast will be compressed as the X-ray is taken, and the technician will take two flat images per breast.
A radiologist will interpret the exam and summarize the results. The screening frequency generally depends on patient age and risk factors, with increased examinations for higher-risk patients. Mammogram screenings help identify breast abnormalities, and are generally recommended between ages 40 and 74.
Digital breast tomosynthesis (DBT/3-D mammography)
This advanced type of mammogram relies on low-dose X-rays and a computer reconstruction which creates 3-D breast images. Traditional mammograms use 2-D images that may hide some abnormal tissue if it overlaps with normal tissue in the picture. This 3-D DBT technology allows the radiologist to view the breast in layers or slices, rather than as single images. It can be used for both screening mammography and for those with symptoms. An advantage is that it’s been shown to have higher accuracy and fewer false positive rates, no matter the level of breast density (dense breast tissue can be harder to assess). However, it uses a higher radiation dose than standard mammography, is more expensive and can take longer to interpret.
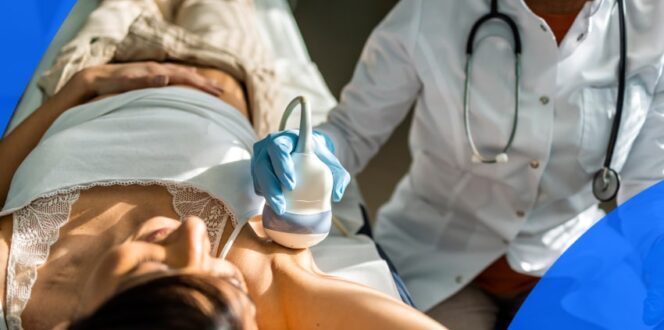
Breast ultrasound
An ultrasound relies on sound waves and echoes, not radiation, to create pictures that may show breast changes or masses. That includes having a greater ability to differentiate between fluid-filled cysts and solid masses. Lumps still may still require additional testing. Ultrasound may be recommended for those with dense breast tissue, as this tissue is harder to see through on mammography, and ultrasound allows the radiologist to view the tissue through multiple angles. Ultrasounds are not recommended as a stand-alone breast screening tool, but as a supplemental or follow-up tool.
Breast magnetic resonance imaging (MRI)
Breast MRIs also do not use radiation, but instead rely on magnets and radio waves to create pictures of the internal breast tissue. It may be recommended for those at high risk of breast cancer, along with a mammogram. It’s also useful for patients with breast implants, as they can obstruct views in traditional mammograms.
Like an ultrasound, breast MRIs are not used as a solo screening test, as mammograms may find some cancers missed by MRI. A breast MRI is a more involved exam, as it requires the use of contrast dye injected in your vein. Another downside of breast MRI is that it may find more false positives than mammograms – tissue that may not actually be breast cancer, but should be tested just in case. Those with false positives may end up needing biopsies. For this reason, an MRI is not used as a screening tool for those with average breast cancer risk. It may be recommended if a person has suspicious findings on exam or from symptoms, and the initial mammogram and breast ultrasound don’t show clear findings.
Newer screening tools
There are some screening tools that are less popular and not accepted yet as standard. That means not all radiology offices offer them and they may not be covered by insurance. While there are many being investigated, here are a few you may have heard about.
Thermography
This screening tool measures the person’s skin temperature with a specialized camera to determine if there may be cancer cells growing in the breast. The thermographic image may show “hot spots” in a different color than the tissue around it. Any tissue with an inflammatory response will be seen as a “hot spot,” making this a less specific and telling exam. If someone has a hot spot, they may be sent back for a mammogram.
Molecular breast imaging (MBI)
MBI uses nuclear medicine imaging, meaning a radiotracer is injected into the person’s blood, to provide high-resolution functional breast tissue images. It may be used as a follow-up for findings like a breast lump or abnormal mammogram. It can also be used if a person is already diagnosed with breast cancer, to understand the extent of the disease.
Getting my results
Turnaround times for the final results can vary widely depending on the facility and your doctor’s availability. Often, patients wait a week or more and receive their results during a follow-up appointment. With PocketHealth, you don’t have to wait as long—your results are available securely as soon as they’re uploaded, allowing you to review them often before your follow-up visit. PocketHealth is also useful for future breast exams, as providing past imaging to the radiologist for comparison can make it easier for them to interpret any changes.
Understanding my results
Although your doctor will provide an explanation of your results, PocketHealth often allows you to access your imaging and report before your follow-up appointment. It’s common to find the medical terminology somewhat confusing, but Report Reader helps you to better understand your report by offering clear, straightforward definitions for medical terms—simply tap or click on any underlined words to reveal their meaning.
Take control of your breast health journey
Given the routine nature of breast imaging, tracking changes over time is essential. Having secure access to all your imaging records in one place allows you to be actively involved in your health journey. You can compare breast changes, send records to other medical providers, and even print and store these reports for your own use. For Ruth, a breast cancer survivor, access to her past breast imaging through PocketHealth helped her reclaim her power. “For me, a lot of it is about control. I want to feel like I’m in control of my health.”
Another tool for your breast health is MyCare Navigator, which provides personalized insights to your health and identifies any recommended follow-up steps. This feature can also generate individualized questions to ask your doctor based on the findings in your report, ensuring you make the most of your consultation.
Published: April 5, 2023
Trusted by more than 800+ hospitals and clinics.