Preparing for an MRI: What to Wear, What to Avoid and Other Tips
July 25, 2024
Read More
A mammogram is a type of X-ray with a low dose of concentrated radiation that monitors changes in breast tissue and is used in breast cancer screening. Mammograms are an excellent preventative measure, often detecting signs of cancer very early, before other symptoms arise. The U.S. Preventative Services Task Force (USPSTF) draft recommends that all women should begin regular mammogram screenings every other year at age 40.
In recent years, 3D mammograms have become available. Also called digital breast tomosynthesis (DBT), 3D mammograms are more accurate than traditional digital mammograms when it comes to diagnosing the earliest signs of breast cancer, especially in dense breasts. In this article, we’ll examine:
A mammogram is an X-ray that uses a very low radiation dose to examine breast tissue. These X-ray images can reveal any abnormal changes before they can be felt in a traditional breast exam. Regular 2D mammograms take two images, one each from the top and the side.
In a 3D mammogram, the X-ray moves in an arc over the breast, taking multiple pictures of the breast from several different angles. Those multiple images or slices, are combined together, providing a more complete view of the breast and making it easier to spot any irregularities.
3D mammograms are highly effective screening mammograms. A 2023 study of more than 1 million women showed that 3D mammograms led both to a higher rate of cancer detection and a lower rate of recalls for further imaging.
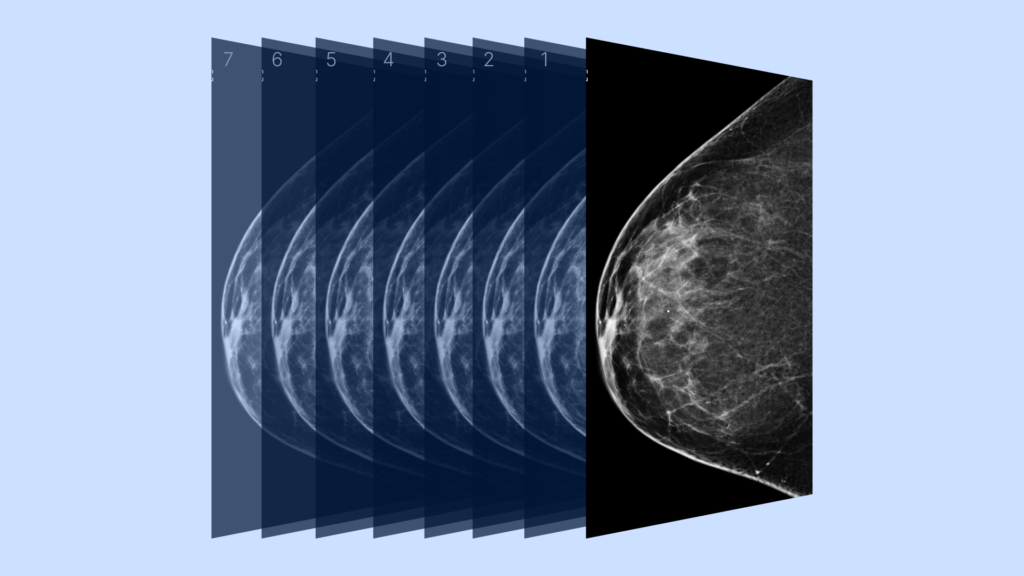
A simplified example of how a 3D mammogram image is built using many image slices taken at different angles, sourced from the National Cancer Institute via National Institutes of Health Image Gallery.
A traditional 2D mammogram provides 2 images of each breast. 3D mammograms provide hundreds of thinly sliced images. Those slices are brought together to create a highly detailed 3D view of the whole breast.
Mammograms are also the only way to assess breast density. 3D mammograms are more effective for dense breasts because physicians can see the dense areas from several different angles.
A traditional 2D mammogram presents two overlapping images. That overlap can obscure potential abnormalities, causing them to be missed at the earliest stages. It’s also possible for overlapping tissue to make benign spots look abnormal, which then requires you to have further imaging done for clarification.
3D mammograms feel like 2D mammograms. In both, your breast is compressed by a clear plate against the X-ray platform and pressure is applied while the X-ray images are taken. That pressure can feel uncomfortable, but it’s necessary to improve image clarity.
3D mammograms take a little longer than traditional mammograms, so the pressure will last several more seconds. It’s important to keep the technologist appraised of your level of discomfort.
There are several reasons someone may choose the 3D option over traditional digital 2D mammograms, including:
Breast density refers to the type and composition of your breast tissue. Dense breasts contain more fibrous and glandular tissue than fatty tissue. Dense breasts are both normal and common, but increased density can obscure images on a regular mammogram. Both cancer and dense breast tissue look white in mammogram images.
Radiologists determine your breast density with mammograms. There are 4 categories:
Breast density is a risk factor for breast cancer. Women with category D density are 4-6 times more likely to develop cancer than people with breasts in the least dense category (less than 25% dense tissue).
Several factors affect breast density, including:
According to this 2023 study, 3D mammograms detect cancer in 5.3 out of 1000 cases, whereas traditional mammograms found cancer in 4.5 out of 1000. That’s a significant difference when it comes to early detection and treatment. Studies have also shown that 3D mammograms detect more kinds of cancer than regular 2D mammograms.
Medical bodies suggest different starting ages, but in 2023, the USPSTF issued a draft recommendation that women start regular screening mammograms every other year beginning at age 40. At 55, you can scan every year in the U.S.
Should you have a family health history of breast cancer, you should begin your screening sooner, and consider both mammograms and MRIs. Always discuss your risk factors with your physician so you can explore the best scan options for your particular needs.
As with all medical procedures, there are pros and cons when getting a 3D mammogram.
Pros
Cons
While a 3D mammogram only requires a short appointment, there are some steps you can take to prepare in advance:
The imaging clinic or department will provide wipes to clean up after your screening, but you may wish to pack deodorant or antiperspirant to bring with you to wear after the appointment. Also, if you are concerned about pain during your appointment, ask your doctor if over-the-counter medication can help reduce discomfort.
Your mammogram technician cannot answer questions about the results of your 3D mammogram. But you can ask questions about the process and procedure, like:
The technologist will send your images to the radiologist, who will compile and interpret the images before sending the full report to your physician. At your follow-up appointment, you can ask more specific questions, such as:
When your 3D mammogram is complete, you can access your images and report through PocketHealth, often before your follow-up appointment with your primary practitioner. Access your records here.
PocketHealth allows you to access, view and store your medical images and health information all in one secure location. You can also use PocketHealth to share images.
Mammography reports are technical documents with complex terminology. PocketHealth Report Reader makes it easy to understand terms in your mammogram report and also highlights any follow-up recommendations, so you can be confident and informed when speaking to your doctor at your mammogram follow-up appointment.
Doctors use mammograms to check for changes and abnormalities in breast tissue. Not all of these are signs of cancer, indeed, many are fairly common. The main changes mammograms scan for are:
In a normal breast image, the background will be black while the breast tissue shows up in shades of gray. Dense tissue and glands will be white, whereas abnormalities like the ones listed above will have unique appearances. For example:
Some of these abnormalities will suggest further testing, which might include another mammogram or a biopsy.
Doctors use a standard vocabulary to describe mammogram results, called the Breast Imaging Reporting and Data System (BI-RADS). BI-RADS has 7 numbered categories.
Regular mammograms are vital for breast cancer detection and prevention. 3D mammograms take many more images than traditional 2D mammograms, which are then combined to create a highly detailed view of breast composition and health.
Mammograms of all types have life-saving potential since they can detect signs of breast cancer before you can feel them. Discuss 3D mammography with your physician to see if it’s the right choice for you. It’s important to stay both informed and proactive when it comes to maintaining your breast health.
Learn more about how to use PocketHealth to access and share your 3D mammogram records.